Expanding care for everyone, everywhere.
Choose from two versatile handheld ultrasound solutions that enable quick and convenient whole-body assessments without compromising on image quality.
3 Year Warranty | Starting at $4,855
Frequently asked questions
Innovation in handheld ultrasound is revolutionizing the use of ultrasound by healthcare professionals and helping to enable more personalized care for patients worldwide.
Pocket-sized handheld ultrasound provides clinicians with a tool to complement the physical exam for focused assessments at the point-of-care.
Handheld ultrasound provides a unique value as an easy-to-use, lightweight, and portable ultrasound tool clinicians can have literally on hand to evaluate and triage patients, enabling them to get answers quickly to help accelerate diagnoses and treatment decisions.
Handheld ultrasound can help improve healthcare outcomes and potentially lower costs by reducing patient wait times and offering a more efficient workflow. It supports increased confidence by supplementing the information gathered throughout the clinical evaluation. Can improve practice management, patient follow-up and referrals to specialists, or in emergencies can help avoid unnecessary referrals and long wait times for additional care.
The use of handheld ultrasound as part of the physical exam may improve patient care. Handheld ultrasound is valuable in enabling clinicians to see what they could only feel or hear at the point-of-care prior to the handheld ultrasound exam.
Delivering information at the point-of-care for decision-making, handheld ultrasound helps clinicians optimize healthcare operations, services, and experience.
Handheld ultrasound may present the opportunity to help you engage patients, which is why physicians are evaluating adding it to their practices. Enhancing clinical relationships requires not only better communication skills, but also tools that close the gap between diagnosis and patient understanding through a more educational and interactive experience. Portable technology, such as Vscan Air handheld ultrasound, helps patients see what their doctors see, and provides more precise information, like the location of an issue. Having another diagnostic tool is appealing to providers looking to improve patient care.
According to the Journal of Ultrasound in Medicine, “By implementing pocket-size ultrasound examinations that took less than 11 minutes to the usual care, we corrected, verified or added important diagnoses in more than 1 of 3 emergency medical admissions. Point of care examinations with a pocket-size imaging device increased medical residents’ diagnostic accuracy and capability.”
Adding a handheld ultrasound exam may also pave the way for rapid diagnosis during a regular doctor’s visit. During an appointment, you may make an immediate decision whether your patient needs to see a specialist and may fast-track needed therapy.
Yes! Vscan Air CL and Vscan Air SL probes pair with the Vscan Air app which is user-validated to be intuitive and easy to use. User support tools on our Vscan Air support web portal provide online services to enhance the Vscan Air experience – from product information to video tutorials to clinical and service support.
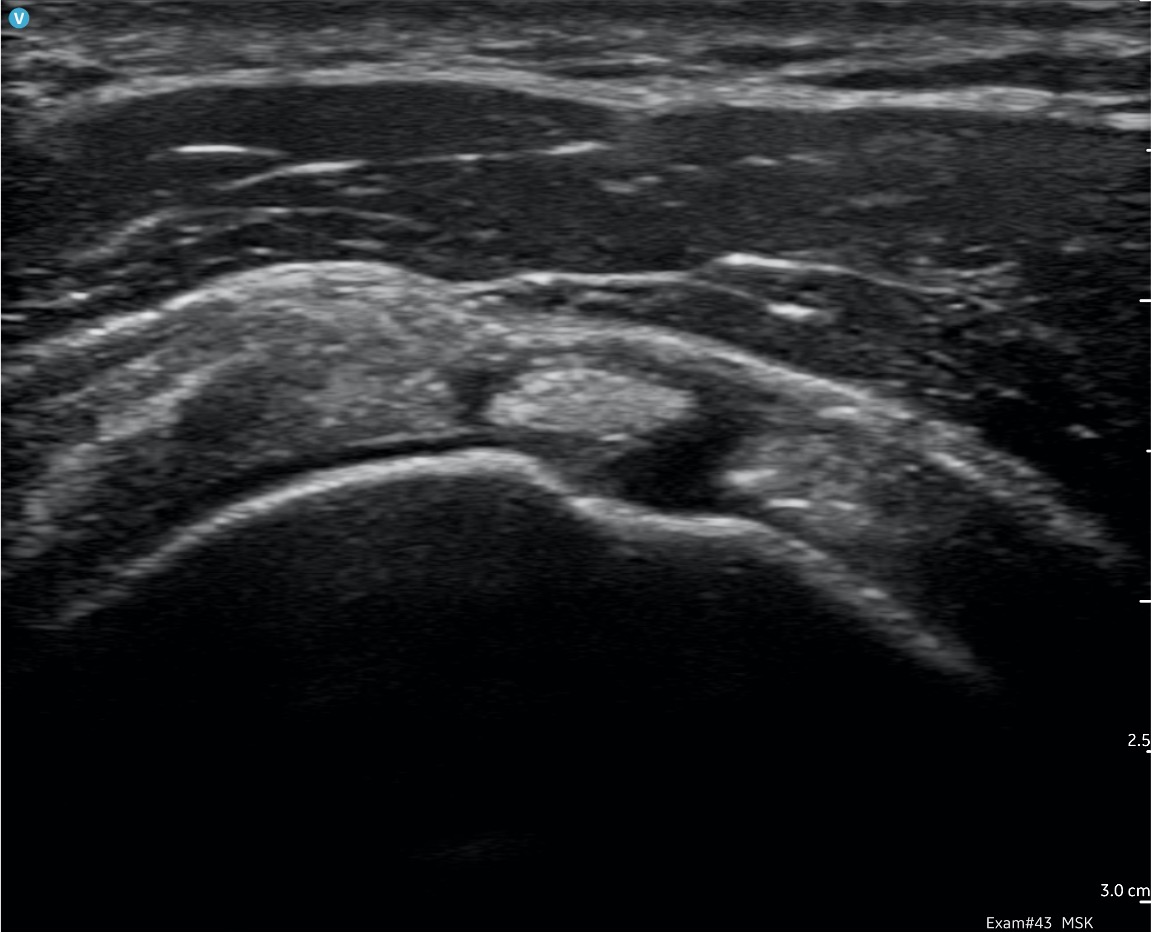
B-mode: Black/white imaging – black-and-white mode for displaying anatomy in two dimensions in real time
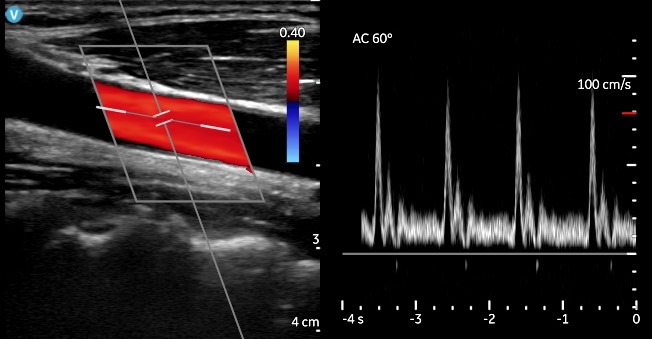
Color Doppler: Color flow – color-coded overlay for real-time blood flow imaging
PW: Pulsed wave spectral Doppler – displays speed and direction of blood flow allowing velocity measurements
M-Mode: Motion mode – displays tissue motion over time (along one direction as indicated by M-mode cursor)
Yes, Vscan Air handheld ultrasound comes with a 3-year standard warranty and the product is backed with local reliable service, education tools and online resources.
Yes, both Vscan Air SL and CL probes use GE HealthCare’s industry-leading dual-probe (2-in-1) technology enabling you to scan patients effortlessly without switching probes between, or during, exams. Complete both shallow and deep ultrasound scans with one probe.
The Vscan Air SL is a flexible, wireless dual-probe with sector phased array and linear array transducers. The Vscan Air CL is a wireless, dual probe with curved array and linear array transducers
